Pain During Periods: When Should It Not Be Ignored?
Most women have been told at some point that painful periods are just part of life. And while some discomfort during a cycle is genuinely common, there is a point where period pain stops being something to simply push through — and starts being something worth talking to a doctor about.
This piece is here to help you understand that difference. Not to alarm you, but to give you a clearer sense of what is within the expected range, and what deserves a proper evaluation.
The Short Answer
Period pain that is mild, lasts a day or two, and does not stop you from going about your day is usually not a cause for concern. But pain that is severe enough to affect your sleep, your work, your studies, or your ability to care for your home especially when it comes alongside other symptoms is not something you should simply accept. It is worth having checked.
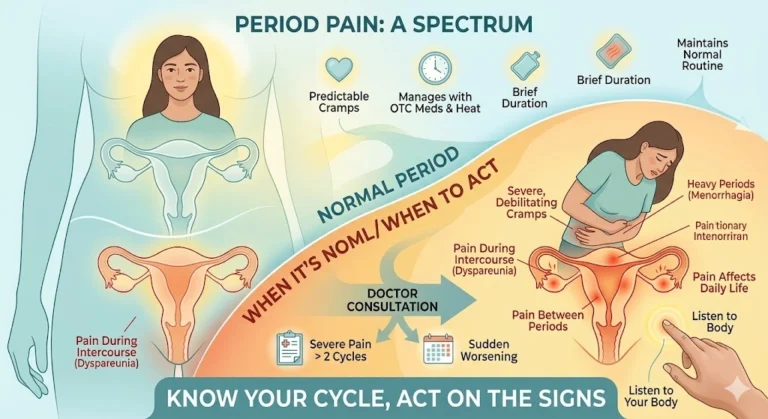
"It's Normal" — But Is It, Really?
There is a particular kind of quiet that many women carry around period pain. They have been told it is normal. Their mothers were told the same. So they take a painkiller, put a hot water bottle on their abdomen, and wait it out.
And sometimes, that is entirely appropriate. Mild cramping in the first day or two of a cycle, caused by the uterus contracting to shed its lining, is genuinely common. Doctors call this primary dysmenorrhoea, which simply means period pain that is not linked to any underlying condition.
But “common” does not always mean “nothing to worry about.” When women describe pain that leaves them curled up in bed, unable to attend class or a work meeting, or needing multiple strong painkillers just to function that is not something to be dismissed. That is a signal worth taking seriously.
The problem is that many women have spent years, sometimes a decade or more, assuming their severe cramps are just how their body works. By the time they see a doctor, there is often an underlying reason that has been quietly present for a long time.
What Kind of Period Pain Is More Expected?
Pain that tends to be within the typical range
– Mild to moderate cramping in the lower abdomen, starting just before or at the beginning of a period
– Discomfort that peaks in the first one to two days and then gradually eases
– Pain that responds reasonably well to a regular painkiller or heat
– A general feeling of heaviness or bloating
– Some lower back ache
This kind of pain, while uncomfortable, usually does not significantly disrupt daily activity. You may feel off, but you can manage.
Pain that may be more concerning
– Pain that is severe enough to keep you in bed or stop you from functioning
– Cramping that starts several days before your period even begins
– Pain that gets worse over time — each cycle more difficult than the last
– Pelvic pain that is present outside of your period as well
– Pain during or after intercourse
– Pain that does not respond to usual painkillers
If any of these sound familiar, it is worth speaking with a gynecologist — not because something is definitely wrong, but because you deserve to know what is actually going on.
When Period Pain Starts Affecting Daily Life
This is perhaps the most important question to ask yourself: Is this pain changing how I live?
Missing school. Taking days off work. Cancelling plans. Not being able to cook, clean, or manage the house. Lying in bed because there is genuinely no other option. These are not signs of being dramatic or having a low pain threshold. They are signs that something may be worth investigating.
A lot of women in our part of the world push through this quietly — trying home remedies, relying on strong painkillers month after month, or simply convincing themselves that it will get better on its own. Sometimes it does. But often, it does not. And the longer an underlying cause goes unaddressed, the more it can affect quality of life.
If your periods are regularly taking a toll on you in a way that feels disproportionate, please do not normalise it on your own. Contact Dr, Sajida Guftaar today!

Symptoms Alongside Period Pain That Should Not Be Ignored
Pain alone tells us something. But pain combined with other symptoms can tell us more. Here are some things that, when they accompany period pain, warrant a proper evaluation:
Heavy bleeding
Soaking through a pad or tampon every hour or two, or passing large clots, alongside severe pain is not typical.
Vomiting or nausea
Some nausea during periods can happen, but vomiting that is difficult to control, especially with intense pain, needs attention.
Dizziness or faintness
feeling like you might pass out during a painful period, or actually losing consciousness, should be assessed promptly.
Irregular or very delayed periods alongside pain
if your cycle is already unpredictable and your pain is severe, there may be a hormonal or structural reason behind both.
Pain between periods or during intimacy
pelvic pain that is not limited to your cycle can sometimes point toward conditions like endometriosis or an ovarian cyst that warrants evaluation.
Bloating or abdominal fullness outside your cycle
Combined with pelvic pain, this is something worth mentioning to a doctor.
Some Possible Reasons Severe Period Pain Happens
If a doctor suspects that your pain is more than simple cramping, there are several conditions that may be explored. Here is a brief, plain-language explanation of the more common ones:
Endometriosis
Tissue similar to the uterine lining grows in other areas of the pelvis. It responds to the hormonal cycle just as the uterine lining does, which is why it causes significant pain around the time of a period — and sometimes outside of it.
Fibroids
Non-cancerous growths within or around the uterus that can cause heavier periods and more intense cramping. They are more common than many women realise.
Ovarian cysts
fluid-filled sacs on the ovaries. Many resolve on their own and cause no symptoms. But some cysts can cause significant pelvic pain, particularly if they are large or have ruptured.
Adenomyosis
condition where the uterine lining grows into the muscular wall of the uterus itself. Women with this often describe a deep, heavy, relentless kind of period pain.
Hormonal imbalance
Hormones regulate the entire menstrual cycle. When they are out of balance, periods can become more painful, more erratic, or more disruptive in ways that go beyond ordinary cramping.
Pelvic inflammatory disease (PID)
An infection affecting the reproductive organs that can cause significant pain during periods and at other times. It requires proper treatment.
None of these diagnoses are made through reading an article. A proper evaluation by a gynecologist is the only way to know what is actually going on.
What a Doctor May Ask or Check
If you visit a gynecologist about period pain, you do not need to worry about the appointment being intimidating. A good evaluation is usually quite straightforward.
The doctor will typically want to understand your symptoms in more detail — when the pain starts, how long it lasts, how severe it feels, whether it has changed over time, and what other symptoms accompany it. They will ask about your menstrual history, including how regular your cycle is and what your flow is like.
A physical examination may be recommended, along with a pelvic ultrasound, which is often the first investigation used to check the uterus and ovaries. Blood tests may also be suggested, especially if hormonal imbalance is a possibility.
The process is not complicated. It is just about building a clear picture of what is happening so that the right guidance can be given.
When Urgent Review Is Needed
Most period pain — even significant period pain — is not a medical emergency. But there are certain situations where you should seek prompt medical attention rather than waiting for a routine appointment:
– Sudden, severe pelvic or abdominal pain that is different from your usual period pain
– Pain accompanied by a high fever
– Vomiting that you cannot control
– Feeling faint or losing consciousness
– Heavy bleeding that is soaking through multiple pads in a short period of time
– Pain that continues to worsen despite taking painkillers
These situations need to be assessed without delay.
Faq's
Is severe period pain always caused by hormones?
Not always. While hormonal changes do drive the normal process of menstruation, severe pain is often linked to structural conditions like endometriosis, fibroids, or adenomyosis — or to infections affecting the reproductive organs. Hormonal imbalance can certainly play a role, but a proper evaluation helps identify the actual cause rather than assuming.
Can ovarian cysts cause painful periods?
Yes, they can particularly if a cyst is large, or if it has ruptured. Many ovarian cysts cause no symptoms at all and resolve without treatment. But some do cause significant pelvic pain, and this pain can be worse around the time of a period. An ultrasound is usually the first step in assessing whether a cyst is present and what kind it is.
When should I get an ultrasound for period pain?
If your period pain is severe, worsening over time, affecting your daily life, or accompanied by other symptoms such as irregular cycles, pain during intimacy, or pelvic discomfort outside your cycle — an ultrasound is a reasonable and commonly recommended first investigation. Your doctor will advise based on your specific situation.
Is it normal for period pain to cause vomiting or faintness?
Mild nausea during a period can happen. But vomiting that is difficult to control, or feeling faint or actually fainting, is not within the expected range. These symptoms alongside severe pain should be evaluated by a doctor, as they may indicate a condition that needs attention.
Can severe, untreated period pain affect fertility later?
It depends on the underlying cause. Period pain itself does not damage fertility. But some of the conditions that cause severe period pain — such as endometriosis or pelvic inflammatory disease — can affect the reproductive organs over time if left unaddressed. This is one of the reasons early evaluation matters. Treatment options exist, and catching something earlier generally makes management more straightforward.
A Final Thought
Period pain is one of those things that women often learn to minimise — because they have been told to, because others around them seem to manage, or because it feels like something to be quietly endured rather than spoken about.
But your body communicating through pain is worth listening to. Not with panic, but with attention. If something feels wrong, or simply feels like more than it should, you are entitled to have it looked at by someone who can actually assess it properly.
A visit to a gynecologist is not an overreaction. It is sensible, practical care — and often, it brings a great deal of clarity and relief.
