Normal Delivery vs C-Section: How Doctors Decide What Is Safer*
Every pregnancy carries its own story. And almost every pregnant woman — especially in the months leading up to her due date — starts wondering the same thing: Will I have a normal delivery, or will I need a C-section? Which one is better? Who decides?
These are completely fair questions. And the fact that you are asking them means you are thinking carefully about your own health and your baby’s wellbeing — which is exactly the right instinct.
This post is not here to push one option over the other. It is here to explain how doctors actually think through this decision, what factors matter, and why there is often no single right answer that applies to every pregnancy.
The Short Answer
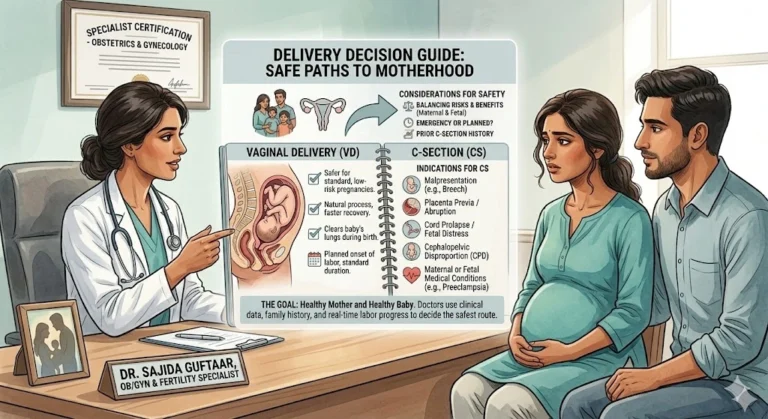
Doctors do not choose between normal delivery and C-section based on preference. The decision is based on what is safest for the mother and the baby at that point in the pregnancy.
Normal delivery is the natural process, and when conditions are suitable, it is generally the first option considered. A C-section is a major surgical procedure — not a shortcut, not a luxury — and it is recommended when a vaginal delivery carries higher risk than surgery.
The final plan is shaped by a combination of factors: the mother’s health, the baby’s position and condition, how the pregnancy has progressed, and sometimes, what happens during labor itself.
Why Families Often Oversimplify This Decision
It is very common to hear opinions from family members, friends, or neighbors about which delivery type is “better.” Some families fear surgery and assume normal delivery is always the goal. Others, perhaps influenced by previous experiences, assume a C-section is cleaner or easier. Neither is universally true.
The real challenge is that this decision is not one-size-fits-all. Two women at the same stage of pregnancy, with similar due dates, might have very different delivery plans — and both plans can be medically correct for their individual situation.
Comparing your delivery plan to someone else’s experience often creates unnecessary anxiety. What your doctor recommends for you is based on your specific pregnancy — not on general rules or popular opinion.
When Normal Delivery Is Usually Encouraged
When a pregnancy is progressing well, normal delivery is typically the goal most doctors work toward. This is not just about tradition — vaginal delivery generally involves a shorter recovery time, a lower risk of surgical complications, and a smoother transition for both mother and baby in most uncomplicated cases.
Conditions That Support Normal Delivery
A normal delivery is usually considered appropriate when:
– The baby is positioned head-down (vertex position) in the final weeks
– The mother’s pelvis is adequate for the baby to pass through
– The placenta is not covering the cervix
– There are no significant medical conditions that would make labor risky
– The baby is showing healthy signs throughout pregnancy
– Labor progresses at a reasonable pace
When these factors are in place and labor begins naturally or is safely induced, the plan is typically to allow vaginal delivery to proceed, with close monitoring throughout.
When a C-Section May Be the Safer Choice
A C-section is not a failure. It is a medical option that, in certain situations, genuinely protects the life of the mother, the baby, or both. Doctors do not recommend surgery lightly — and when they do, it is for specific, clear reasons.
Situations Where C-Section Is Often Recommended
A planned C-section may be advised when:
– The baby is in a breech position (feet or bottom first) and has not turned by the due date
– The placenta is positioned low, covering the cervix — a condition called placenta previa
– The mother has certain medical conditions such as severe hypertension, some heart conditions, or active infections that make vaginal birth risky
– The baby is very large relative to the mother’s pelvis
– There are signs of fetal distress that suggest the baby cannot tolerate labor
– A previous uterine surgery has been done in a way that increases the risk of uterine rupture during labor
An emergency C-section may also become necessary during labor, even after a vaginal delivery was planned. This can happen if the baby’s heart rate drops in a concerning way, if labor stops progressing, or if the cord comes out before the baby.
What Doctors Are Actually Looking At
When a gynecologist or obstetrician is assessing the safest delivery route, they are weighing multiple things together — not just one factor in isolation.
The Factors That Shape the Decision
- Maternal health history: Conditions like diabetes, blood pressure, previous surgeries, or uterine fibroids all matter.
- Baby’s position and size: The baby’s presentation, estimated weight, and growth pattern are assessed through ultrasound in the later weeks.
- Placenta location: Where the placenta is sitting can directly affect whether vaginal birth is safe.
- Amniotic fluid levels: Too little or too much fluid can signal problems that need careful management.
- Gestational age: How far along the pregnancy is affects everything from risk to readiness.
- Progress of labor: If labor begins but does not progress — even after interventions — this changes the picture.
- Signs from the baby during labor: Continuous monitoring during labor gives the medical team real-time information about how the baby is coping.
What If You Have Had a C-Section Before?
This is one of the most common questions women ask — and one where assumptions can cause unnecessary worry.
Having had one previous C-section does not automatically mean every future pregnancy must end in surgery. In many cases, a vaginal birth after cesarean — often called VBAC — is considered a safe option, depending on several factors.
These include the type of incision used in the previous surgery, how long ago it was, how the current pregnancy is progressing, and whether there are any complications this time around. Not every woman is a candidate for VBAC, but many are — and that is something worth discussing with your doctor rather than assuming either way.
Equally, if you have had two or more C-sections, your doctor will review your uterine history carefully before making any recommendation about how to proceed.
Why the Delivery Plan May Change Near Labor
Many women receive a tentative plan earlier in pregnancy — and then find that it shifts in the final weeks or even during labor. This can feel unsettling, but it is actually a sign that the medical team is responding to what is actually happening, not just following a fixed script.
Conditions change. A baby that was well-positioned at 34 weeks may not turn head-down by 38 weeks. A pregnancy that looked straightforward may develop a complication that was not present earlier. Labor that starts on its own may slow down or create unexpected pressure on the baby.
The final delivery plan is always meant to be flexible, because the goal — a safe outcome for mother and baby — sometimes requires last-minute decisions.
If your plan changes, ask your doctor to explain why. A good explanation will help you understand the reasoning and feel more confident about the decision being made.
What to Discuss With Your Doctor Before Your Due Date
You do not need to wait until something feels wrong to ask your doctor about your delivery plan. These are questions worth raising in your third trimester, ideally in the final 6 to 8 weeks.
Questions Worth Asking
– Based on my pregnancy so far, what delivery option are you currently leaning toward — and why?
– Is there anything in my health history that could affect this plan?
– What position is the baby in right now, and does that matter at this stage?
– If a normal delivery is planned, what would cause you to recommend a C-section instead?
– If a C-section is planned, what would make you reconsider?
– What is your approach to pain management during labor?
– At what point would you consider inducing labor?
– If I need an emergency C-section, how would that be handled?
You do not need to memorize these questions. Just come to your appointment willing to have an open, honest conversation about how things are going.
Faq's
Is normal delivery always better than a C-section?
Not always. Normal delivery is the preferred option when it is safe, because it usually involves less recovery time and fewer surgical risks. But when vaginal birth poses a greater risk to the mother or the baby, a C-section is the better and safer choice. The goal is always a safe outcome — not achieving a particular method of delivery.
If I had a C-section before, does every future delivery have to be surgical?
Not necessarily. Many women are able to have a vaginal birth after a previous C-section, depending on the type of incision, the time since the surgery, and how the current pregnancy is going. This is something to discuss specifically with your doctor, because the answer depends on your individual history.
When is a planned C-section the safer option?
A planned C-section is usually recommended when there is a known condition that makes vaginal birth risky — such as the baby being in a breech position, the placenta covering the cervix, or certain maternal health conditions. In these situations, planning ahead gives the surgical team time to prepare properly, which generally leads to better outcomes.
Can the delivery plan change after it has already been decided?
Yes, and this is normal. Pregnancy and labor are dynamic. Even a well-planned delivery can change course based on what happens in the final weeks or during labor itself. If your plan changes, ask your doctor to walk you through the reason — it is always better to understand than to feel confused or anxious.
What should I bring up with my doctor in the last month of pregnancy?
In the final few weeks, it is a good time to confirm the baby’s position, understand the current plan, ask what would cause a change in that plan, and clarify where and how you should go when labor begins. Being informed helps you feel prepared rather than caught off guard.
Final Thoughts
Most women who think about this question are not really asking which delivery method is “better” in the abstract. They are asking: Will I be okay? Will my baby be okay? That is the question your doctor is working to answer throughout your entire pregnancy. The goal is not a particular delivery experience. The goal is a healthy mother and a healthy baby — and whatever path leads there most safely is the right one for you.
If you have questions or concerns about your own pregnancy and delivery options, speaking with a trusted gynecologist is always the most reliable starting point.
